Resultat

Linnékliniken fortsatt i topp!
De senaste öppna jämförelserna från Q-IVF finns nu publicerade. Q-IVF är Sveriges nationella kvalitetsregister för IVF. För att ta del av resultaten klicka här.
Allmänt
Sedan starten 1990 är över 12 000 barn födda efter olika typer av behandlingar vid Carl von Linné Kliniken. Pågående graviditeter är hela tiden minst 300 st. Detta gör kliniken till en av dem i Norden som hjälpt flest par att få barn. En anledning till detta är en hög lyckandegrad under alla år.
Nya fina resultat i KUPP 2023
KUPP - kvalitet ur patientens perspektiv - mäter hur patienterna upplever vården på landets IVF-kliniker. Vi har i alla år legat högt i dessa mätningar. Vi är stolta över att vi i den senaste undersökningen från vårvintern 2023 ligger högt i alla kategorier.
Vilken klinik har Sveriges bästa IVF-resultat? Se Q-IVF 2023
Färska siffror från landets alla kliniker under 2019-2021 (juni) finns nu inrapporterade till Q-IVF. Nedan visas i staplar resultaten för olika åldersgrupper. Se även på q-ivf!
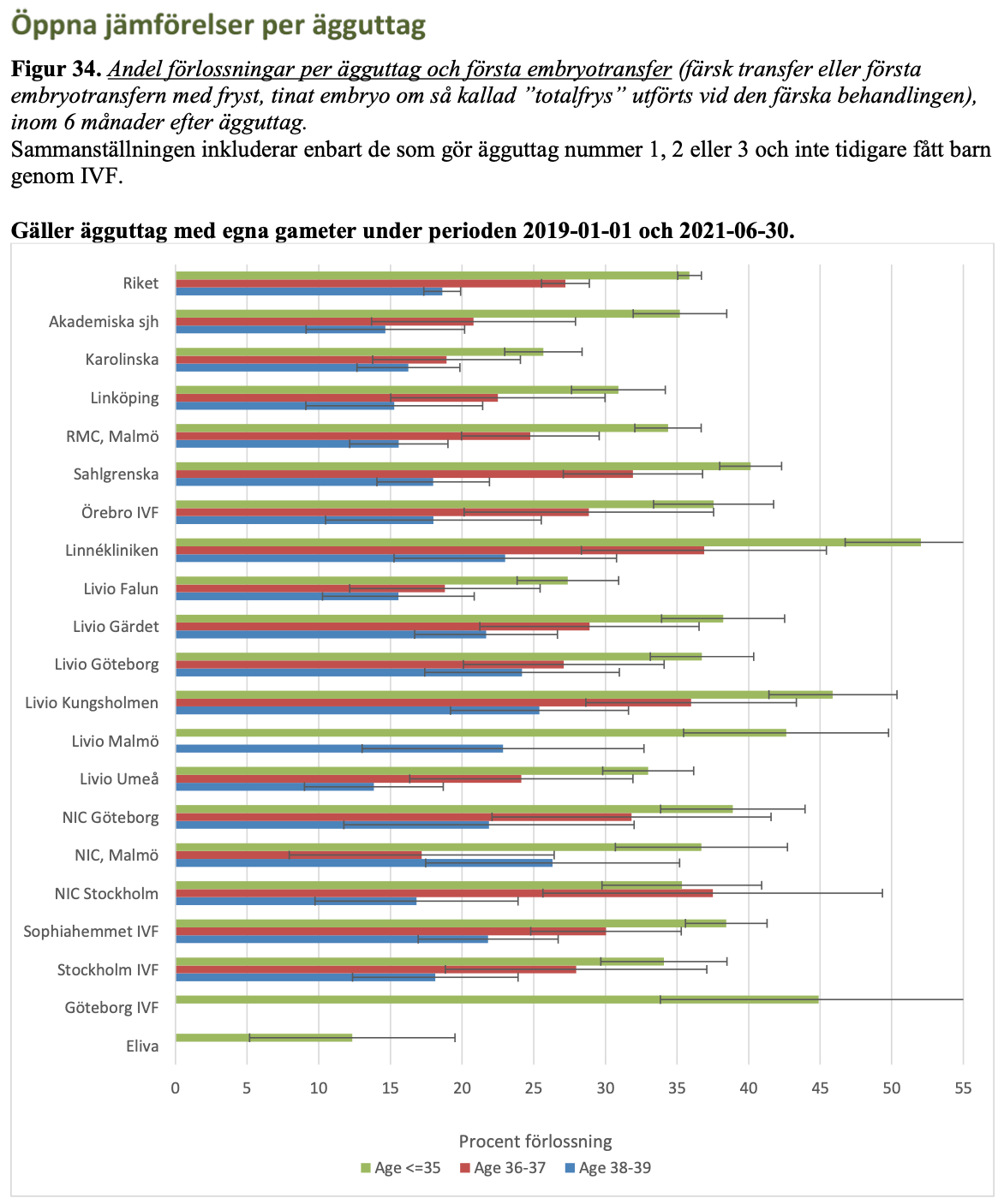
Carl von Linnéklinikens resultat i topp
Mycket goda resultat
Stadigt bättre resultat är en trend vi noterat de senaste åren. Orsaken är små men viktiga förbättringar inom hela den komplicerade IVF-processen. Vår egenutvecklade prognosmodell har visat sig ovärderlig för denna utveckling.
Med hjälp av den kan vi enkelt undersöka både nya och etablerade metoder, som t ex olika hormonstimuleringar för patienter i olika åldrar och med olika äggreserv, olika labmetoder m m och jämföra med det ”facit” som modellen ger oss. På så vis kan mindre effektiva metoder bytas mot mer effektiva metoder. Vi kan alltså se vilka faktorer som är av betydelse och vilka som är betydelselösa och anpassa behandlingen därefter.
Du kan läsa mer om prognosmodellen här och du kan också se på filmen på första sidan.
Färska återföringar 2017-2022
| ålder | antal
embryoåterföringar | antal
gravida | gravida, %* | pågående
graviditeter/ förlösta, %* |
| <35 | 1190 | 613 | 52% | 44% |
| 35–37 | 713 | 299 | 42% | 32% |
| 38–39 | 505 | 167 | 33% | 23% |
| 40–42 | 793 | 214 | 27% | 15% |
*Procenttalen är per embryoåterföring.
Med graviditet avses klinisk graviditet där graviditet påvisats med ultraljud. Positiva test med åtföljande snar blödning ("biokemisk graviditet") är alltså inte medräknade.
Frysåterföringar 2017-2022
| ålder | antal
embryoåterföringar | antal
gravida | gravida, %** | pågående
graviditeter/ förlösta, %** |
| <35 | 1486 | 806 | 54% | 46% |
| 35-37 | 731 | 342 | 47% | 36% |
| 38-39 | 448 | 201 | 45% | 33% |
| 40-42 | 479 | 171 | 36% | 21% |
**Procenttalen är per embryoåterföring.
Med graviditet avses klinisk graviditet där graviditet påvisats med ultraljud. Positiva test med åtföljande snar blödning ("biokemisk graviditet") är alltså inte medräknade.
Resultatsiffror kan skilja sig beroende på om man anger utfall per startad behandling eller per embryoåterföring. Av olika skäl förekommer att behandlingar bryts strax efter att stimuleringen startat, eller att embryoåterföring inte kan göras p g a att det saknas embryon som lämpar sig för återföring. En annan viktig anledning till att återföring ibland inte görs i färsk behandling är de fall där man fryst alla tillgängliga embryon p g a risk för farlig överstimulering. Det medför att färre fullföljer än startar en behandling. Andelen gravida per embryoåterföring bli därför större, jämfört med utfallet per startad behandling eller per ägguthämtning.
Prognosfaktorer
Sedan flera år har vi systematiskt och i samarbete med Uppsala Universitet undersökt faktorer hos embryon som påverkar chansen för graviditet. Vi har även systematiskt registrerat en mängd faktorer hos de par vi behandlat. Under det senaste året har utvärderingar av alla dessa faktorer gjorts med avancerad statistisk metodik. Detta har lett fram till två viktiga resultat. Det första är att vi bättre kan avgöra vilket embryo som har störst chans att resultera i graviditet. Ett andra viktigt resultat är att vi nu bättre kan ge det enskilda paret en prognos för hur stor chansen är att en IVF-behandling lyckas i just deras fall.
Ålderns betydelse
Den enskilt viktigaste faktorn som avgör om man kan lyckas eller ej med IVF är kvinnans ålder. Man räknar med att den naturliga fruktsamheten redan vid 36-37 år har avtagit ordentligt jämfört med i 20-årsåldern och detta avspeglar sig även i IVF resultaten. Vad som sker är en försämring av äggkvaliteten, vilket leder till färre graviditeter och fler missfall. Vi tillämpar en åldersgräns på 42 år för kvinnan för IVF med egna ägg. Orsaken är att våra liksom andras erfarenheter entydigt visar att behandlingar över den åldern resulterar i mycket få graviditeter.
Individuella skillnader
Även om åldern i sig är den viktigaste faktorn för chansen att lyckas, så finns det en ganska stor variation mellan olika kvinnor i de åldrar där reslutaten börjar sjunka. Vi arbetar vetenskapligt med att bedöma olika kvinnors förutsättningar och har idag stor erfarenhet för att kunna ge mer individuell rådgivning till paren. Basen är dels en noggrann undersökning av patientens äggstockar med ultraljud, dels hormonprover som kan tas före behandlingsstart.
Vid ultraljudsundersökningen räknas antalet omogna äggblåsor i äggstockarna och äggstockarnas storlek skattas. Våra resultat talar för att graviditetschanserna är större ju fler omogna äggblåsor och ju större äggstockar patienten har. På så sätt kan en kvinna i 39-40 årsåldern med "bra" äggstockar ha lika stor chans att lyckas med behandlingen som en kvinna som är betydligt yngre men med mindre välförsedda äggstockar. Den här bedömningen görs vid parets första besök hos doktorn och ingår i den vanliga gynekologiska undersökningen.
Hormonprov som kompletterar ultraljudsundersökningen är fr a Antimüllerskt hormon, AMH, samt ibland hypofyshormonerna FSH och LH, vilka mäts i blodet i tidig menscykel. Hormonvärdena, särskilt AMH, har visat sig vara ett bra mått på kvarvarande mängd ägg i äggstockarna och på så sätt finns ett samband med vilken chans paret har att lyckas. Det är bl.a. dessa fynd som används i den prognosmodell som tidigare omnämnts. Ett annat enkelt mått på den s k äggreserven är hur långa menscykler kvinnan normalt har (långa cykler bättre än korta).
Antal embryon för återföring?
Det har med åren skett en stor förändring i rutinen hur många embryon som sätts in i livmodern. Vi följer Socialstyrelsens direktiv att sätta in ett embryo i flertalet fall för att hålla antalet tvillinggraviditeter på ett minimum. Tidigare (fram till början av 2000-talet) återfördes mer eller mindre regelmässigt två embryon. Bakgrunden till ett-embryo-policyn är att uppföljande studier visat en klart ökad risk för barnen om de föds som tvilling jämfört med s.k. singelgraviditet (hänvisning ex. Torbjörn Bergh och medförfattare, Lancet, vol 354, 1999. Socialstyrelsens rapport 2000:4). Exempelvis är risken för CP-skada hos en tvilling fyra gånger högre än hos ett barn som varit ensamt i livmodern. (Risksiffrorna skiljer sig dock inte mot risken för tvillingar som tillkommit utan behandling.)
Numer (2020-talet) återför vi ett (1) embryo i nästan alla behandlingar, i synnerhet om det görs återföring av blastocyst (5-dagarsembryo) vilket är det allra vanligaste (läs med under IVF och Ett eller två embryon?).
Vid ev återföring dag 2 efter ägguttag avgör våra unika matematiska modeller om ett eller två embryon kan återföras. Med hjälp av dessa kan vi enkelt avgöra när man faktiskt vid återföring dag 2 ökar graviditetschansen mer markant genom att återföra två ägg, utan att tvillingrisken samtidigt blir hög. Och när ett embryo ger nästan lika hög graviditetschans som två, men utan en stor tvillingrisk. Se även under Ett eller två embryon?
Hur ändras resultaten när vi strävar att få färre tvillinggraviditeter?
Med hjälp av vår databaserade prognos- och urvalsmodell fortsatte resultaten vid tvådagarsåterföringar, som tidigare var rutin, att vara glädjande höga. Den s.k. implantationsfrekvensen (chansen för ett enskilt embryo att utvecklas till graviditet) blev högre än tidigare år då två embryon sattes in. Det beror på att vi allt oftare hittat rätt embryo att återföra. Antalet behandlingar där embryon kan sparas och frysas ökade markant. Tillsammans gjorde detta att chansen att bli gravid efter en ägguttagning (inkl resultat från ev återföring av frysta-tinade embryon) var oförändrat på den höga nivå som vi vant oss vid tidigare då två embryon i princip alltid sattes tillbaka. Detta trots att vi samtidigt sänkte andelen tvillingförlossningar till ca 2 % (från tidigare 28 %), vilket var den lägsta nivån i landet. Viktigast är att detta medförde en dramatisk sänkning av andelen födda barn med låg födelsevikt (viktig riskfaktor för CP-skada). Denna andel liksom antalet barn som dog före eller i anslutning till förlossningen sjönk markant. Dessa siffror kom att bli helt i nivå med dem som man finner då graviditeten uppkommit utan behandling.
Läs mer om den här dramatiska förbättringen av resultaten under rubriken Vetenskap. Vill du få en uppfattning om vilka chanser just du skulle ha vid behandling hos oss? Kontakta oss. Oftast kan en enkel ultraljudsundersökning och ett par blodprover ge en god uppfattning om det.
Numer (2020-talet) görs i regel återföring av blastocyst dag 5 och då också nästan uteslutande med ett embryo. Att odla till blastocyst hjälper oss vid urvalet av embryo för återföring. Embryot måste också gå vidare till detta stadium för att det alls ska kunna bli en graviditet, oavsett om det sker i livmodern efter återföring dag 2 eller i laboratoriet vid vidareodling.
Vad innebär blastocystodling?
En av de metoder som används för att välja bäst embryo att återföra, innebär förlängd odling i värmeskåp i fem dagar i stället för två eller tre. Helst ska då ett embryo utvecklas till en s.k. blastocyst.
De embryon som inte har möjlighet ("kapacitet") att dela sig vidare efter de allra första dagarna stannar i utvecklingen under den förlängda odlingen, och endast de mest livskraftiga blir kvar. En orsak till detta är att inte alla embryon är av fullgod kvalitet, och ju längre embryon odlas, desto tydligare avslöjar sig de med sämre chans.
Som rutin odlar vi numer vidare till s k blastocyst i alla behandlingar. Man kan också sätta embryo åter redan på andra eller tredje dagen. För att det ska bli en graviditet, dvs för att embryot ska implantera ("fästa") och kunna utvecklas vidare i livmodern, måste dock embryot dela sig vidare och bli en blastocyst. Läs mer här.
Vi föredrar alltså att se att embryot delar sig vidare innan återföringen görs. Dels hjälper det oss att välja rätt embryo ifall det finns flera att välja mellan. Utöver det ger det oss också en del information om parets förutsättningar vilket kan vara till hjälp vid kommande rådgivning ifall behandlingen inte lyckas.
Vi använder för dag-2-embryon vår unika embryoscoring och prediktionsmodell och har då också möjlighet att objektivt skatta risken för en tvillinggraviditet för att avgöra om det kan vara aktuellt att erbjuda två embryon åter. Vid återföring av blastocyst är dock en åter regel och det är mycket sällan två åter kan övervägas.
Det skrivs mycket på nätet
Vi vet av erfarenhet att det förekommer mängder av uppgifter på chatsidorna på nätet om olika åtgärder, behandlingar eller faktorer som sägs kunna öka chansen till graviditet för paret. Det är dock viktigt att läsa sådana uppgifter med ett mycket kritiskt sinne. De flesta av dessa uppgifter kan ej bekräftas i kontrollerade vetenskapliga studier. Lyckandefrekvensen vid en klinik kan variera från en period till en annan utan att man säkert vet varför, dessutom är det stora individuella skillnader mellan olika pars förutsättningar. Det är därför bara om man gör undersökningar på ett riktigt vetenskapligt sätt som man kan värdera om en metod är bättre än en annan.
Undersökning på instagram 2023-01-31.
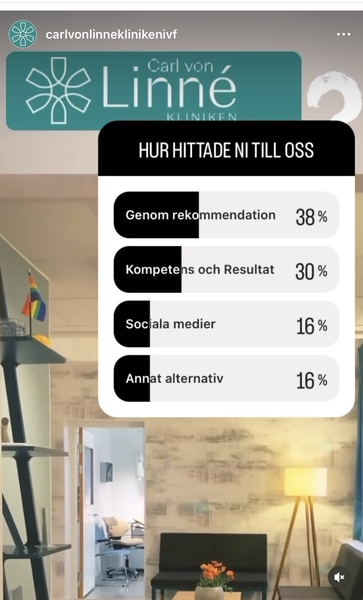 Undersökning på Instagram om varför patienter väljer Linnékliniken.
Undersökning på Instagram om varför patienter väljer Linnékliniken.